
Generic cancer drugs fail quality tests at alarming rate, investigation shows
www.statnews.com
June 30, 2025, 1:47 p.m.
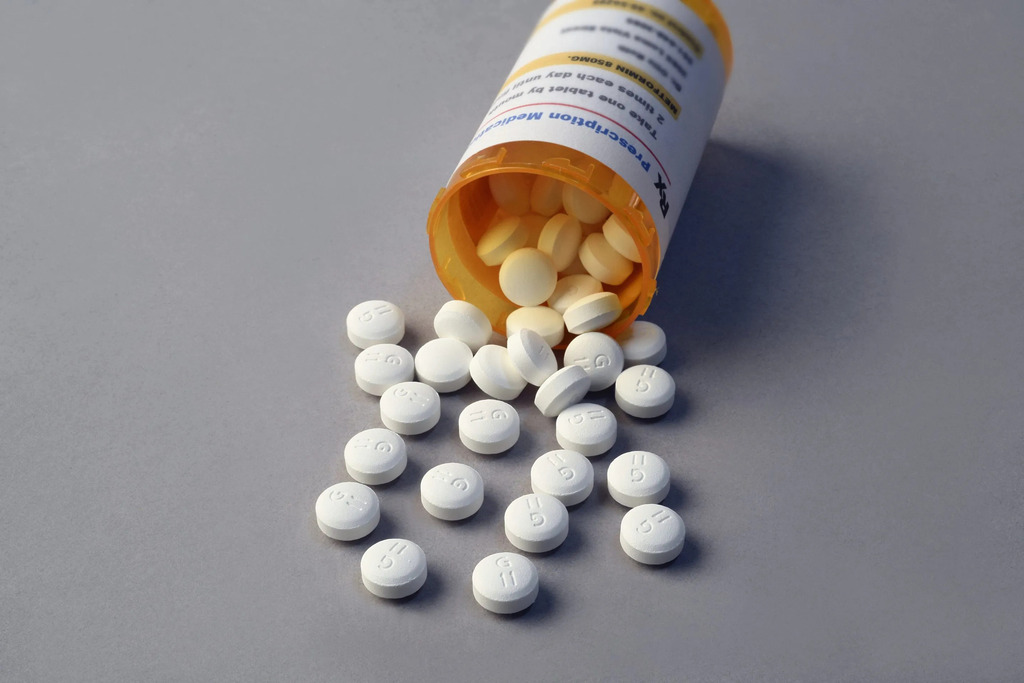
The variance found in the levels of active ingredients was alarming. In some cases, pills from the same blister pack contained different amounts. These findings expose huge holes in the global safety nets intended to prevent manufacturers from cutting corners to boost profits, and to protect patients from bad drugs. All the while, patients and governments with stretched resources are paying the price for drugs that don’t work.
Share on
Can people with type 2 diabetes live longer than those without? A comparison of mortality in people initiated with metformin or sulphonylurea monotherapy and matched, non-diabetic controls
dom-pubs.pericles-prod.literatumonline.com
June 25, 2025, 11:25 a.m.
Patients with type 2 diabetes initiated with metformin monotherapy had longer survival than did matched, non-diabetic controls. Those treated with sulphonylurea had markedly reduced survival compared with both matched controls and those receiving metformin monotherapy. This supports the position of metformin as first-line therapy and implies that metformin may confer benefit in non-diabetes. Sulphonylurea remains a concern.
Share on

How Weight-Loss Drugs Blew Out the U.S. Trade Deficit
www.wsj.com
June 22, 2025, 12:58 p.m.
Shipments have propelled Ireland, a country of 5.4 million, to the second-largest goods-trade imbalance with the U.S., behind China.
Share on

Ageing Population: A Catalyst for Healthcare Innovation
www.bsigroup.com
June 14, 2025, 3:19 p.m.
The considerations posed by an ageing population are indeed substantial, yet shifting demographics also make clear the opportunity to enhance patient outcomes and improve people’s health and lives represented by transformative advancements in healthcare technology. The increasing demand for care has ignited a surge in innovation across healthcare system. From artificial intelligence (AI) and robotics to telemedicine and wearables, there is opportunity to harness technology to enhance the quality of life for all, including those most in need of healthcare interventions, and to bolster the capacity of healthcare providers.
Share on
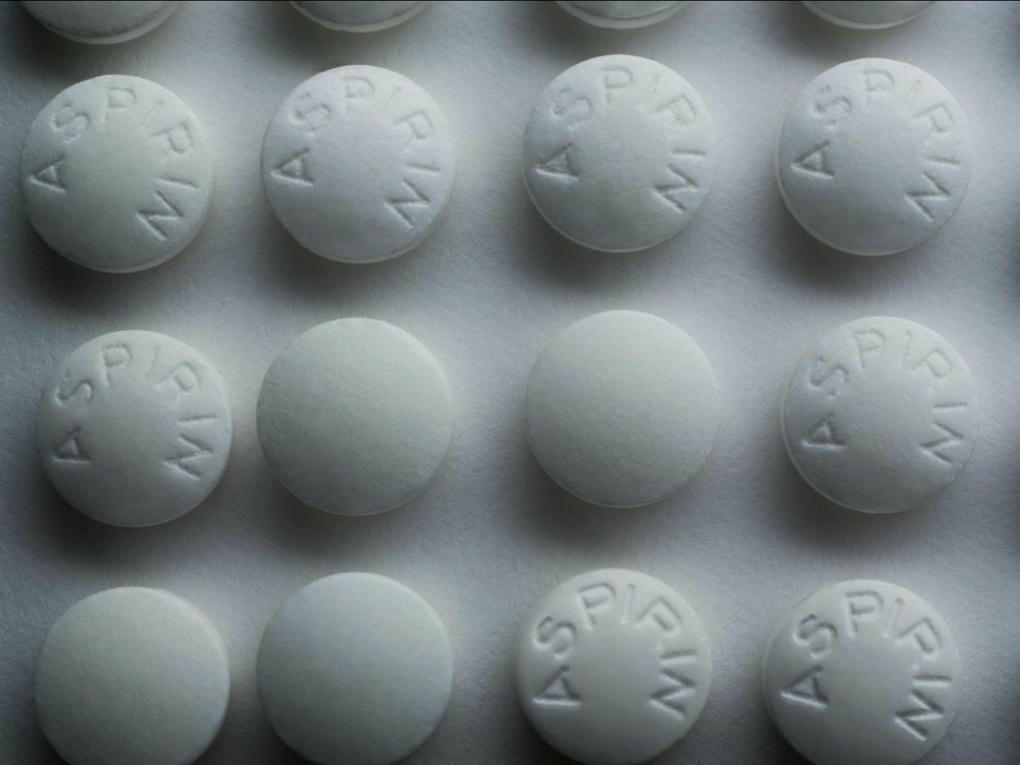
On sait enfin pourquoi l'aspirine prévient les métastases dans certains cancers
www.sciencesetavenir.fr
June 11, 2025, 7:47 p.m.
Si l'aspirine diminue fortement le risque de certains cancers de se répandre sous forme de métastases, c'est grâce à un gène particulier, inactivé dans certaines cellules immunitaires, ont découvert par hasard des chercheurs.
Share on

Artificial Blood That Could Work for All Blood Types in Trials
www.newsweek.com
June 9, 2025, 10:33 a.m.
The World Health Organization estimates that more than 118 million blood donations are collected each year—with 40 percent coming from high-income countries, home to 16 percent of the world's population. This means a large portion of the global population has limited access to blood transfusion treatment. Universal artificial blood could reduce preventable deaths in injury, surgery and childbirth—settings where supply mismatches or stockouts cost millions of lives annually in low-income nations alone.
Share on

Liver Abscess Risk After Biliary Stents in Pancreatic Cancer
bioengineer.org
June 3, 2025, 8:19 a.m.
In the realm of pancreatic cancer treatment, biliary stent placement has emerged as a vital intervention, offering relief for patients suffering from obstructive jaundice. This procedure, while life-prolonging and often essential, carries with it a significant risk: the development of pyogenic liver abscesses (PLA), a severe and potentially fatal complication. Recent retrospective research brings to light critical insights concerning the incidence, pathology, and management of PLA following biliary stent placement in pancreatic cancer patients, pushing the boundaries of our understanding and underscoring the urgency of heightened clinical vigilance.
Share on
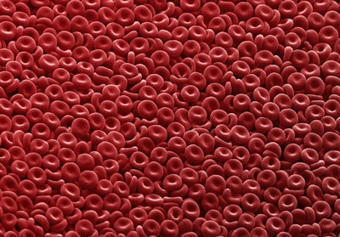
Japanese Scientists Created Universal Artificial Blood
www.healthcarepackaging.com
May 18, 2025, 8:39 p.m.
The artificial blood could be a game-changer for blood transfusions as it can safely be administered to all patients regardless of blood type.
Share on

Une nouvelle génération de CAR-T armés pour surmonter les échecs thérapeutiques
www.caducee.net
May 11, 2025, 4:33 p.m.
Une thérapie cellulaire de nouvelle génération, enrichie en interleukine-18, montre une efficacité notable chez des patients atteints de lymphome B réfractaire, déjà traités par CAR-T anti-CD19. Un espoir renouvelé face aux impasses thérapeutiques.
Share on

Enhanced CAR T cell therapy offers new strategy for lymphoma
medicalxpress.com
May 11, 2025, 4:32 p.m.
A next-generation "armored" CAR T cell therapy showed promising results in a small study of patients whose B-cell lymphomas continued to resist multiple rounds of other cancer treatments, including commercially available CAR T cell therapies. The new therapy diminished cancer in 81% of patients and resulted in complete remission in 52%, with some of the earliest patients treated experiencing durable remission for two years or more.
Share on

Digital Health : La digitalisation, incontournable pour la modernisation du secteur pharmaceutique
www.lavieeco.com
April 21, 2025, 4:13 p.m.
L’essor de l’intelligence artificielle, du Big Data, de la blockchain et de la télémédecine ouvre de nouvelles perspectives pour une médecine plus personnalisée, efficace et accessible. La digitalisation n’est plus une option mais une nécessité stratégique pour améliorer l’efficacité des soins.
Share on

Roche stops pivotal TIGIT trial as Keytruda lands knockout blow
www.fiercebiotech.com
April 19, 2025, 4:18 p.m.
Keytruda has beaten Roche’s TIGIT drug candidate at the first interim analysis of a phase 2/3 lung cancer trial, prompting the Swiss drugmaker to stop the study and consider changes to the broader program.
Share on
GSK Grabs Rights to Technology That Gets Drugs Across the Blood-Brain Barrier
medcitynews.com
April 19, 2025, 4:15 p.m.
GSK is licensing an ABL Bio technology that yields bispecific antibodies engineered to leverage a certain transmembrane receptor to cross the blood-brain barrier to treat neurodegeneration. GSK is already partnered with Alector, which has monoclonal antibodies in clinical development for Alzheimer’s disease.
Share on

Medication Adherence and Deprescribing Programs Aren’t Enough for Today’s Polypharmacy Patients
medcitynews.com
April 19, 2025, 4:13 p.m.
By moving beyond adherence and drug interactions to a holistic, outcomes-driven approach, health systems and providers can redefine how medication is used — not as a rigid protocol but as a dynamic, patient-centered tool for achieving better health.
Share on

Pfizer Stops Work on Oral GLP-1 Obesity Drug After Safety Signal Surfaces in Clinical Trial
medcitynews.com
April 19, 2025, 4:12 p.m.
Pfizer said a patient dosed with danuglipron developed potential drug-induced liver injury. Pfizer is stopping further work on this program, a move that comes nearly two years after it discontinued development of a different obesity drug due to liver safety signals in a clinical trial.
Share on

How the Health Sector Can Change Vaccine Messaging Amid Rising Anti-Vaccine Sentiment
medcitynews.com
April 19, 2025, 4:10 p.m.
Robert F. Kennedy Jr.’s rise to become secretary of the Department of Health and Human Services has some concerned that anti-vaccine policies are coming. If the nation’s top public health agency pulls support of vaccination, other healthcare stakeholders will need to step up to fill the vaccine messaging void.
Share on

DrugOptimal : Une Appli Pour Détecter Les Incompatibilités Médicamenteuses
mesinfos.fr
March 17, 2025, 8:21 a.m.
Créée en 2022, DrugOptimal développe une application logicielle à destination des établissements de santé, et en particulier des infirmiers et les pharmaciens, pour mieux prévenir les risques d'incompatibilités physicochimiques médicamenteuses.
Share on

Revolutionizing Drug Delivery: The Impact of Advanced Materials Science and Technology on Precision Medicine
www.mdpi.com
March 17, 2025, 8:18 a.m.
The integration of advanced materials into drug delivery systems has become the new normal in pharmaceutical science to address the complexity of modern medicine. These innovations have used technologies such as nanocarriers, hydrogels, and bioresponsive polymers to enable precision, efficiency, and superior therapeutic outcomes. Advanced materials have revolutionized drug delivery by improving upon conventional systems, and their application in various fields, including oncology, chronic disease management, and vaccine delivery, has been remarkable.
Share on

Worrying amounts of microplastics found in human brain tissue - how to reduce exposure
www.universal-sci.com
March 4, 2025, 3:26 p.m.
Microplastics are everywhere—in our water, food, and even the air we breathe. A new scientific review highlights a growing concern: microplastics and nanoplastics are accumulating in human brain tissue. Researchers are now investigating what this could mean for brain health and how we can reduce our exposure.
Share on

Takeda's anti-CD38 antibody boosts platelet count in phase 2
www.fiercebiotech.com
March 4, 2025, 3:15 p.m.
Last month, the Japanese pharma deprioritized the development of mezagitamab, also known as TAK-079, in myasthenia gravis and systemic lupus erythematosus as part of a wider pipeline shake-up. But the team said at the time that it was still planning to continue to clinically evaluate the antibody in ITP.
Share on