
Innovative Glioblastoma Immunotherapy Treatment
bookinghealth.com
May 9, 2026, 2:10 p.m.
Glioblastoma (GBM) is known for its aggressive biology. It can also demonstrate significant resistance to standard therapies. Therefore, before discussing "why" patients should consider immunotherapy (IT) for GBM, we would like to explain the unique challenges that glioblastoma cells can pose; the reasons why current GBM treatments often fail; and how utilizing the body's immune defenses can potentially increase survival of patients with brain tumors.
Share on
Recent Developments in Lipid Nanoparticle-Mediated Delivery of ...
link.springer.com
May 8, 2026, 10:51 p.m.
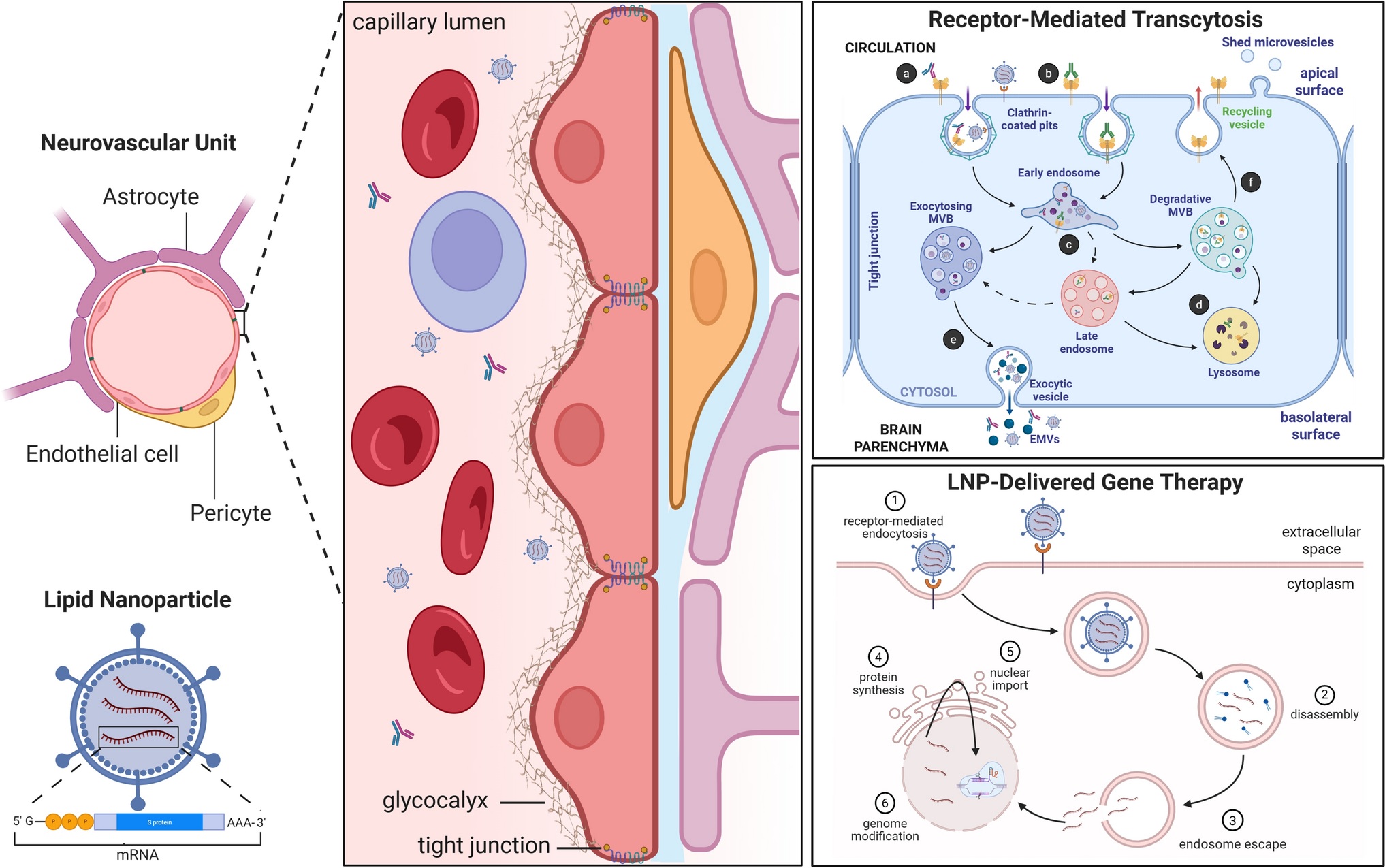
Lipid nanoparticles (LNPs) have emerged as a promising delivery platform for complex therapeutics targeting the central nervous system, addressing significant challenges posed by the blood–brain barrier. While peripheral administration of biotherapeutics such as antibodies, immunotherapeutics, and gene therapies has traditionally been limited by anatomical barriers, recent advances in LNP technology offer compelling alternatives to viral vectors. By leveraging receptor-mediated transcytosis mechanisms and functionalizing LNPs with blood–brain barrier-penetrant moieties, researchers are successfully enabling CNS delivery of various therapeutic modalities, including messenger RNA, small interfering RNA, and antisense oligonucleotides. These innovations, validated through preclinical models and emerging clinical studies, represent a transformative approach to treating neurological indications and expanding the therapeutic potential of advanced biotherapeutics.
Share on

IL-6 underlies microenvironment immunosuppression and ... - PubMed
pubmed.ncbi.nlm.nih.gov
May 8, 2026, 10:51 p.m.
Interleukin-6 (IL-6) plays a critical role in creating an immunosuppressive microenvironment that contributes to treatment resistance in glioblastoma, one of the most aggressive primary brain tumors. This research identifies IL-6 as a key mediator of immune evasion mechanisms, highlighting its potential as a therapeutic target. Understanding the molecular pathways through which IL-6 promotes immunosuppression and therapy resistance offers promising avenues for developing combination treatment strategies that could enhance patient outcomes in glioblastoma management.
Share on

The Science of Glioblastoma Brain Cancer - Emotiv
www.emotiv.com
May 8, 2026, 10:51 p.m.
Emotiv provides advanced brain data measurement hardware and software solutions designed to enhance scientific understanding of glioblastoma, a highly aggressive form of brain cancer. The platform leverages cutting-edge neurotechnology to capture and analyze brain activity patterns, enabling researchers to gain deeper insights into disease mechanisms and treatment responses. By combining non-invasive brain imaging with sophisticated data analytics, Emotiv's solutions support the development of more targeted therapeutic interventions and personalized treatment strategies. These innovations represent a significant advancement in oncology research, offering hope for improved patient outcomes through better diagnostic and monitoring capabilities in glioblastoma management.
Share on

Accessing CAR-T Therapy for Glioblastoma in China (2026)
www.medbridgenz.com
May 8, 2026, 10:50 p.m.
China has emerged as a leading hub for advanced glioblastoma treatment through CAR-T cell therapy, with over 66 clinical trials launched across major medical institutions between 2022 and 2025. Chinese researchers are pioneering multi-antigen targeting strategies using dual or tri-specific CAR-T cells to overcome tumor resistance, while innovative manufacturing platforms have dramatically reduced production times from weeks to 24-36 hours. Estimated costs for experimental CAR-T therapy in investigator-initiated trials range from $40,000 to $80,000. This represents a significant advancement for glioblastoma patients, as conventional Western treatment protocols yield median overall survival of only 12-15 months initially and 6-8 months upon recurrence. International patients increasingly explore these cutting-edge therapies at JCI-accredited neuro-oncology centers targeting critical antigens such as EGFRvIII and HER2, marking a paradigm shift in neurological oncology treatment options.
Share on
Clinical, molecular, and immunologic determinants of survival in WHO ...
pmc.ncbi.nlm.nih.gov
May 8, 2026, 10:50 p.m.
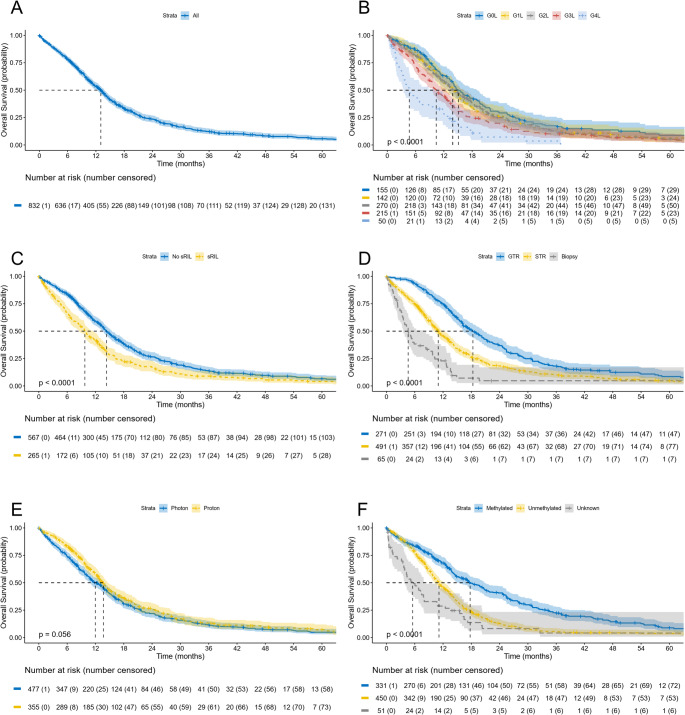
This large real-world cohort study examines the clinical, molecular, and immunologic factors that influence survival outcomes in patients with WHO-defined IDH-wildtype glioblastoma treated with radiotherapy. Conducted by researchers at the University of Pennsylvania's Department of Radiation Oncology, the investigation identifies key prognostic determinants across multiple biological dimensions. By integrating clinical characteristics with molecular profiling and immunologic markers, the study provides comprehensive insights into treatment response and patient prognosis. These findings enhance our understanding of glioblastoma heterogeneity and may inform personalized treatment strategies to optimize radiotherapy outcomes in this aggressive brain tumor population.
Share on

La science du cancer cérébral du glioblastome
www.emotiv.com
May 8, 2026, 5:37 p.m.
Le cancer du cerveau appelé glioblastome, un type de tumeur cérébrale vraiment difficile, pose de sérieux défis aux médecins et aux patients. Il est connu pour être agressif et difficile à traiter, revenant souvent même après un traitement. Cet article examine pourquoi le glioblastome est si difficile à traiter, ce qui le fait fonctionner au niveau cellulaire, et les nouvelles idées que les chercheurs explorent pour le combattre.
Share on

Glioblastoma studies show promise
www.unc.edu
May 8, 2026, 5:36 p.m.
One UNC Healthclinical trialbegun in 2022 intends to evaluate the safety and patients’ toleration of chimeric antigen receptor T-cell therapy. The trial is treating patients whose cancer has not successfully responded to one or more treatments. The CAR-T process involves extracting specific immune cells from patients, engineering the cells in a lab to identify tumor cells displaying a specific molecular target, then re-infusing the cells to fight the patient’s brain tumor. Now programmed to have “chimeric antigen receptors” or CARs, the T-cells latch onto tumor cells and destroy them.
Share on

How the Challenges of Glioblastoma Treatment Highlight New Opportunities for Next-Generation Antibody Therapeutics
www.biopharminternational.com
May 8, 2026, 5:36 p.m.
Blood–brain barrier tight junctions, efflux transporters, and poor tissue diffusion necessitate systemic agents with improved CNS exposure, without relying on infeasible surgical completeness or inconsistent local delivery platforms. Intratumoral heterogeneity and antigen loss drive resistance to single-antigen biologics, supporting multispecific constructs that engage multiple targets and/or recruit effector cells to counter clonal evolution. Immunosuppressive GBM microenvironment limits checkpoint and CAR T efficacy via inhibitory cytokines, Treg activity, and PD-L1 upregulation, motivating therapeutics that locally modulate immune function.
Share on
Nebivolol suppresses glioblastoma progression via dual modulation of mitochondrial metabolism and AKT/mTOR/4EBP1 signaling axis
journals.plos.org
April 27, 2026, 7:50 a.m.
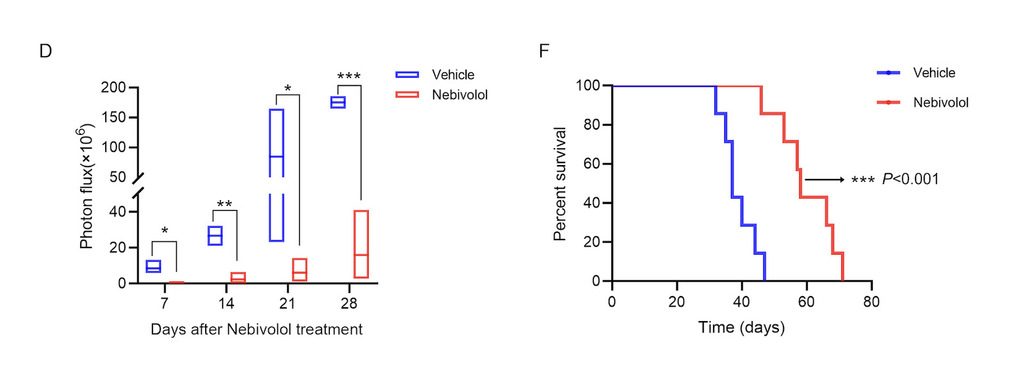
Emerging evidence reveals the pivotal involvement of mitochondrial metabolic dysregulation in glioblastoma (GBM) pathogenesis, considering mitochondrial metabolism as a potential therapeutic target. Nebivolol, a third-generation β-adrenergic receptor antagonist clinically employed in cardiovascular diseases, has recently exhibited notable anti-neoplastic properties. Nevertheless, its therapeutic efficacy and mechanistic underpinnings in GBM remain largely unexplored. In this investigation, we comprehensively assessed the impact of nebivolol on GBM cellular proliferation and elucidated its molecular mechanisms. Our findings revealed that nebivolol markedly suppressed the proliferation and clonogenic abilities of multiple GBM cell lines, concomitant with cell cycle arrest and apoptotic induction.
Share on
New outlook on the diagnosis, treatment and follow-up of childhood-onset craniopharyngioma
www.nature.com
April 18, 2026, 9:21 a.m.
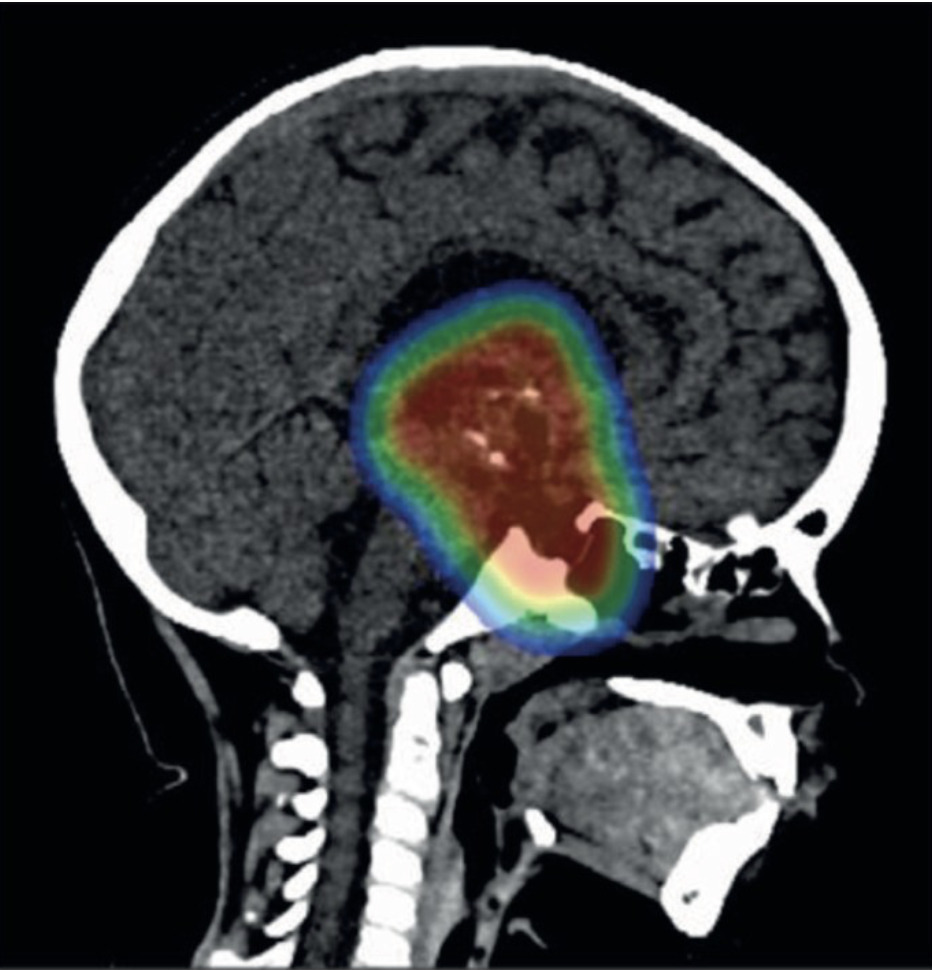
The clinical, neuroradiological and surgical definition of hypothalamic involvement is a fundamental factor related to poor postoperative outcome, progressive obesity and neuropsychological impairment in children after surgical removal of craniopharyngiomaThe previously assumed 'gold-standard' objective of a primary radical removal of the lesion in all cases needs to be replaced with the new paradigm of a limited resection plus focused radiotherapy in patients with craniopharyngioma and hypothalamic lesions

Surface-engineered dual drug-loaded tumor-targeted liposomal nanoparticles to overcome the therapeutic resistance in glioblastoma multiforme
www.nature.com
April 8, 2026, 8:39 p.m.
Glioblastoma (GBM) is the most common high-grade primary malignant brain tumor, characterized by a notably poor prognosis. Current treatments for GBM have shown limited effectiveness in improving patient survival, highlighting the urgent need for effective therapeutic strategies. Combination therapy offers significant potential in overcoming resistance by targeting multiple signaling pathways; however, it often comes with increased toxicity compared to monotherapy. Co-encapsulating multiple therapeutic agents into a tumor-targeted drug delivery platform holds promise for overcoming these limitations and improving treatment outcomes.
Share on

L-RNA Aptamer Enhances Glioblastoma Therapy in GLORIA Trial
bioengineer.org
April 8, 2026, 8:38 p.m.
In an unprecedented advancement in glioblastoma treatment, a groundbreaking phase I/II clinical trial known as GLORIA has unveiled promising results combining L-RNA aptamer-based CXCL12 inhibition with radiotherapy and bevacizumab in newly diagnosed patients. This innovative therapeutic approach targets the molecular microenvironment of glioblastoma, offering renewed hope in a field long hindered by the aggressive nature and poor prognosis of this brain malignancy. The recently expanded trial, detailed in a 2026 publication in Nature Communications by Giordano et al., marks a significant milestone in neuro-oncology, especially by leveraging molecular precision to overcome resistance mechanisms intrinsic to glioblastoma.
Share on

GAD1 Halts Glioblastoma via GSK3β/β-Catenin Pathway
bioengineer.org
March 23, 2026, 10:37 a.m.
In a groundbreaking study set to reshape our understanding of glioblastoma progression, researchers have identified glutamate decarboxylase 1 (GAD1) as a critical suppressor of this aggressive brain tumor through modulation of the GSK3β/β-catenin signaling pathway. Glioblastoma, notorious for its rapid growth and poor prognosis, remains one of the most challenging malignancies to treat effectively. This discovery opens new avenues for therapeutic intervention targeting the molecular underpinnings driving tumor proliferation and invasiveness.
Share on

[64Cu]Cu-Labeled αCD11b Diabody as a Novel PET Tracer for the Detection of Immunosuppression in Glioblastoma
pubs.acs.org
March 16, 2026, 9:51 a.m.
[64Cu]Cu-αCD11b Db is a high-affinity and stable diabody, which can quantify CD11b-positive TAMCs in the tumor microenvironment, particularly when the molar activity of the administered [64Cu]Cu-αCD11b Db is optimized for managing the CD11b antigen sink in the spleen, liver, and bone marrow.
Share on

Dual phagocytosis-checkpoint blockade revitalizes immune surveillance in mouse models of glioblastoma
www.nature.com
March 16, 2026, 9:49 a.m.
Macrophage-mediated phagocytosis of tumor cells elicits potent antitumor immunity. Nonetheless, sole-blockade of the anti-phagocytosis molecule CD47 has yielded insufficient therapeutic outcomes. Here, we report that glioblastoma (GBM) cells expressed abundant levels of phagocytosis checkpoint CD24. We further show that dual blockade of CD24 and CD47 synergistically enhances the pro-phagocytic activity of macrophages, thereby improving tumor antigen cross-presentation and activating the cyclic GMP-AMP synthase–stimulator of interferon genes (cGAS-STING) pathway. This innate immune activation facilitates T cell infiltration into tumors and sensitizes tumors to anti-PD1 therapy, improving survival outcomes in murine GBM models, including immunosuppressive tumors reflecting human GBM-like features. Thus, our results indicate that dual-phagocytosis checkpoint blockade offers a promising therapeutic avenue to potentiate cancer immunotherapy.
Share on

A phase I-II study of niacin in patients with newly diagnosed glioblastoma: safety and interim phase II analysis
link.springer.com
Feb. 16, 2026, 9:56 a.m.
Survival of patients with glioblastoma (GB) treated with standard of care (SOC) surgery, radiotherapy, and temozolomide is 15 months with progression free survival at 6 months (PFS-6 M) of 53.9%. In vivo studies showed increased survival in mice with GB treated with niacin. This is a first in human Phase I-II study aiming to evaluate safety and efficacy of controlled-release niacin (NiacinCRT ™) added to SOC.
Share on

Woman shares unlikely survival journey after migraines led to glioblastoma diagnosis: "I am truly an outlier"
www.cbsnews.com
Feb. 15, 2026, 11 a.m.
Valle said she had no side effects from participating in the trial. Four years after her diagnosis with glioblastoma, she has no evidence of disease. It's a rare positive outcome for a disease that kills most patients within 18 months. "I am truly an outlier," Valle, now 41, said.
Share on
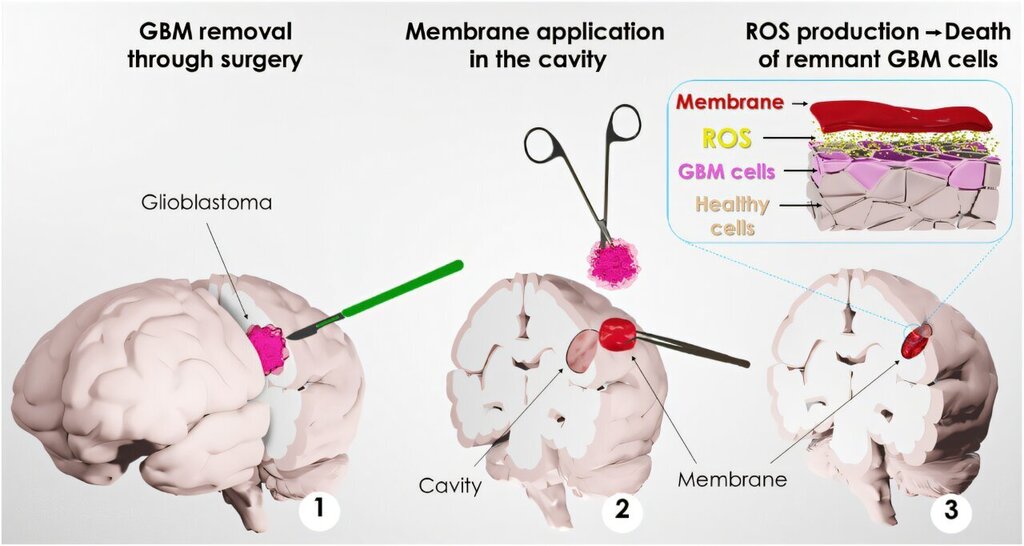
A Mussel-Inspired Bioadhesive Patch to Selectively Kill Glioblastoma Cells
advanced.onlinelibrary.wiley.com
Feb. 9, 2026, 8:13 a.m.
Our work introduces for the first time the use of novel bioinspired membranes designed as a potential patch platform for localized intervention in glioblastoma after surgery, representing a promising advancement in this field. Despite the rapid growth in mussel-inspired research, this work is distinctly innovative. Unlike the common hydrogel and coatings focus, our solid, free-standing bioadhesive membranes could offer a unique solution for glioblastoma treatment. Moreover, their selective toxicity against cancer cells, while sparing healthy astrocytes in vitro, highlights their potential for a novel and targeted application. Our bioinspired membrane addresses critical challenges such as adhesion in humid environments, infection prevention, and biocompatibility. The adhesive properties of the membrane ensure it stays in place, allowing for the sustained delivery of the localized cytotoxic effect to the affected area. This novel approach offers a localized and sustained therapeutic concept based on ROS modulation, that could complement the current glioblastoma treatment paradigm.
Share on

Taming Tumor Chaos: Researchers Uncover Key to Improving Glioblastoma Treatment
neurosciencenews.com
Feb. 2, 2026, 9:48 a.m.
When glioblastoma tumors are treated with chemotherapy, levels of miR-181d drop. This drop amplifies the differences among individual cells within the tumor, thereby allowing more cells to make more MGMT and survive treatment. The research team found that administering miR-181d into the tumor can reduce this effect, making the cancer cells behave more uniformly, and importantly, more likely to respond to chemotherapy.
Share on