
Artificial pancreas under stable pulsatile Model Predictive Control: Including the physical activity effect
www.sciencedirect.com
May 10, 2026, 9:40 a.m.
This paper has presented a comprehensive model of glucose regulation in type 1 diabetes that explicitly integrates physical activity effects into an artificial pancreas system. The proposed pulsatile Zone Model Predictive Control (pZMPC) strategy demonstrates robust performance across challenging scenarios that reflect real-world conditions, including variable exercise intensities, announcement errors, and circadian variations in insulin sensitivity. The integration of physical activity into the control system architecture through a dedicated linear model proves particularly valuable in preventing exercise-induced hypoglycemia while maintaining effective overall glycemic control. Our results quantify the benefits of exercise announcement, showing that when the physical activity event is programmed (i.e., foreseen in advance over the prediction horizon), time-in-range increases and hypoglycemic events decrease compared to non-programmed scenarios.
Share on

New research shows how blood sugar-regulating cells change in ...
www.eurekalert.org
May 9, 2026, 2:02 a.m.
Researchers at Lund University have completed the most comprehensive mapping of the epigenome in pancreatic cells that regulate blood sugar levels. The study, published in Nature Metabolism, examined hundreds of thousands of cells from twenty-four individuals with and without type 2 diabetes. The findings reveal how chemical modifications to DNA alter the activity of insulin-producing beta cells and glucagon-producing alpha cells, demonstrating distinct epigenetic patterns between diabetic and non-diabetic individuals. These discoveries highlight how DNA methylation differences regulate genes essential for insulin and glucagon production, providing valuable insights into the molecular mechanisms underlying type 2 diabetes development.
Share on

Blood Glucose Monitoring - StatPearls - NCBI Bookshelf - NIH
www.ncbi.nlm.nih.gov
May 9, 2026, 2:02 a.m.
Blood glucose monitoring serves as a fundamental component of diabetes management, facilitating the detection of glycemic patterns in response to diet, physical activity, medications, and physiological processes. Accurate and timely glucose assessment is critical, as both elevated and reduced blood glucose levels can precipitate acute, life-threatening emergencies and contribute to long-term microvascular and macrovascular complications. This essential clinical practice enables healthcare providers and patients to optimize therapeutic interventions and maintain glycemic control, directly impacting morbidity and mortality outcomes in diabetic populations.
Share on
Scientists develop a living artificial pancreas that monitors blood sugar ...
okdiario.com
May 9, 2026, 2:02 a.m.
Researchers at Israel's Technion, collaborating with U.S. partners, have developed a groundbreaking living artificial pancreas designed to autonomously monitor blood glucose levels and release insulin without external intervention. The cell-based implant incorporates a protective crystalline shield that defends insulin-producing cells from immune rejection, addressing a critical challenge in transplantation. While current evidence derives from animal studies demonstrating year-long functionality in mice and primates, this innovation promises significant benefits for the estimated 589 million diabetics worldwide. Beyond improved patient care, the technology addresses environmental concerns associated with disposable diabetes management devices. Although cross-species implants still trigger immune responses in primates, this work represents a promising step toward practical clinical applications.
Share on
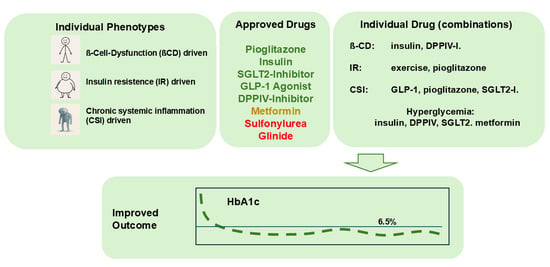
Personalized Diabetes Therapy Part 2—Individual Diabetes ... - MDPI
www.mdpi.com
May 9, 2026, 2:02 a.m.
This article addresses personalized diabetes therapy through an advanced treatment framework termed Standard of Care Plus (SOC+), representing the second installment in a comprehensive series on individualized diabetes management. Building upon functional phenotyping principles established in the first part, this work explores innovative approaches to tailoring therapeutic interventions based on individual patient characteristics and disease presentations. The research contributes to the evolving field of precision medicine by demonstrating how personalized profiling can optimize diabetes treatment outcomes beyond conventional protocols. Published in an open-access format, this study provides significant potential impact for clinicians and researchers seeking to enhance treatment efficacy through individualized, evidence-based strategies.
Share on
Impaired glucose tolerance and mild diabetes induce β-cell ... - Nature
www.nature.com
May 9, 2026, 2:02 a.m.
This study demonstrates that relatively modest elevations in blood glucose of 2-3 millimolar are sufficient to impair pancreatic β-cell function in mice, representing a critical finding for understanding type 2 diabetes progression. The research reveals that chronic mild hyperglycaemia induces significant metabolic changes including altered gene expression, reduced insulin content, decreased metabolic enzyme activity, and compromised mitochondrial function. These observations suggest that β-cell dysfunction occurs early during the prediabetic phase, well before clinical diabetes diagnosis. The findings underscore the importance of therapeutic intervention during the impaired glucose tolerance stage, before severe metabolic deterioration occurs. This work fundamentally advances understanding of how subtle glycaemic changes initiate the gradual decline in insulin-secreting capacity that characterizes type 2 diabetes development.
Share on

Closing in on the Mechanisms of Pulsatile Insulin Secretion
diabetes.diabetesjournals.org
March 18, 2022, 7:21 a.m.
The challenge ahead is to efficiently use our accumulated knowledge of mouse islets to understand the oscillations in the more important (to us) human islets and identify new therapeutic targets that can restore normal pulsatile patterns to patients with type 2 diabetes.

Diabetes: Controlled glucose delivery could restore insulin production
www.medicalnewstoday.com
Oct. 30, 2016, 3:02 p.m.
Type 2 diabetes is characterized by high blood glucose, triggered by reduced production of the hormone insulin. In a new study, researchers reveal how administering controlled pulses of glucose has the potential to restore normal insulin production and prevent the development of type 2 diabetes.
Share on
MAT: A Therapy That Slows and Repairs Diabetic Complications
www.informationaboutdiabetes.com
July 22, 2015, 1:53 a.m.
Metabolic Activation Therapy (MAT), also called cellular activation therapy or pulse insulin therapy, provides diabetic patients with significant symptom improvement. The primary purpose of MAT is to improve the physical and chemical changes in the body that cause diabetic complications.
How does Insulin help in diabetic treatment
thefootballexaminer.com
Oct. 6, 2014, 12:17 p.m.
Insulin is a hormone produced by the beta cells of pancreas. It is released in a pulsatile fashion and plays an important role in the metabolism of carbohydrates and fats and promotes the absorption of glucose from blood to the skeletal muscles and fat tissues.
Share on

Insulin's role in diabetic treatment
www.oaoa.com
Oct. 3, 2014, 12:39 a.m.
Insulin is a hormone produced by the beta cells of pancreas. It is released in a pulsatile fashion and plays an important role in the metabolism of carbohydrates and fats and promotes the absorption of glucose from blood to the skeletal muscles and fat tissues. In a healthy individual, insulin is available within the body in a constant proportion to remove excess glucose from the blood which otherwise would be toxic.
Share on

MAT: A Therapy That Slows and Repairs Diabetic Complications
www.informationaboutdiabetes.com
Sept. 26, 2014, 8:36 a.m.
Metabolic Activation Therapy (MAT), also called cellular activation therapy or pulse insulin therapy, provides diabetic patients with significant symptom improvement. The primary purpose of MAT is to improve the physical and chemical changes in the body that cause diabetic complications.
Share on

Effects of Pulsatile IV Insulin Delivery on Diabetic Retinopathy in Patients With Types 1 and 2 Diabetes Mellitus
www.bioportfolio.com
Aug. 27, 2014, 5:05 p.m.
Diabetic Retinopathy is the leading cause of blindness in the world. Previous studies have documented beneficial effects of physiologic administration of pulsatile insulin on a variety of diabetic complications such as nephropathy, hypertension, glycemic control, etc. Similar pathogenetic mechanisms have been postulated for diabetic retinal disease. This study examines the effect of pulsatile insulin on patients with varying stages of diabetic retinal disease.
Share on

Sugar Diabetes Video
www.salemfreemedclinic.org
Aug. 9, 2014, 9:40 a.m.
Pulsatile Insulin Therapy in Diabetic Patients with Non-healing Wounds. It has been a painful distraction growing in intensity as I age every since. how to control diabetes the natural way glucose levels for diabetes type 2 This ...
Share on
Reversing Lada Diabetes
www.salemfreemedclinic.org
Aug. 9, 2014, 9:39 a.m.
Control of pulsatile insulin secretion in man. Medications Some medications have side effects of raising blood glucose. There are two types of insulin syringes: U-40 (for insulin of the 40 units per cc concentration) and ...
Share on

Hypoglycemia Without Diabetes
www.salemfreemedclinic.org
July 7, 2014, 11 a.m.
Pulsatile insulin sometimes called metabolic activation therapy or cellular activation therapy describes in a literal sense the intravenous injection of insulin in pulses versus continuous infusions. Oatmeal Cherry Cookies. But please at least explain your disagreement.
Share on



